Which Omega-3s Are Beneficial?
Author: Dr. Stephen Chaney
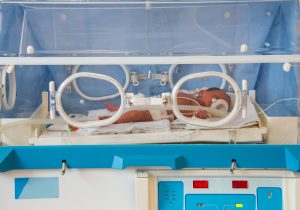 Preterm births (births occurring before 37 weeks) are increasing in this country. Just between 2018 and 2019, the percentage of preterm births increased by 2% to over 10% of all pregnancies. That is a concern because preterm births are associated with an increased risk of:
Preterm births (births occurring before 37 weeks) are increasing in this country. Just between 2018 and 2019, the percentage of preterm births increased by 2% to over 10% of all pregnancies. That is a concern because preterm births are associated with an increased risk of:
- Visual impairment.
- Developmental delays.
- Learning difficulties.
- Problems with normal development of lungs, eyes, and other organs.
Plus, it is expensive to keep premature babies alive. One recent study estimated that reducing the incidence of preterm births by around 50% could reduce health care costs by $6 billion in the United Stated alone.
Of the 10% preterm births, 2.75% of them are early preterm births (births occurring before 34 weeks). Obviously, the risk of health problems and the cost of keeping them alive is greatest for early preterm babies.
We don’t know why preterm births are increasing, but some experts feel it is because in this country:
- More older women are having babies.
- There is increased use of fertility drugs, resulting in multiple babies
Unfortunately, there is no medical standard for identifying pregnancies at risk for preterm birth. Nor is there any agreement around prevention measures for preterm births.
However, recent research has suggested that some premature births may be caused by inadequate omega-3 status in the mother and can be prevented by omega-3 supplementation.
What Do We Know About Omega-3s And Risk Of Preterm Births?
 The role of omega-3s on a healthy pregnancy has been in the news for some time. Claims have been made that omega-3s reduce preterm births, postnatal depression, and improve cognition, IQ, vision, mental focus, language, and behavior in the newborn as they grow.
The role of omega-3s on a healthy pregnancy has been in the news for some time. Claims have been made that omega-3s reduce preterm births, postnatal depression, and improve cognition, IQ, vision, mental focus, language, and behavior in the newborn as they grow.
The problem is that almost all these claims have been called into question by other studies. If you are pregnant or thinking of becoming pregnant, you don’t know what to believe.
Fortunately, a group called the Cochrane Collaboration has recently reviewed these studies. The Cochrane Collaboration consists of 30,000 volunteer scientific experts from across the globe whose sole mission is to analyze the scientific literature and publish reviews of health claims so that health professionals, patients, and policy makers can make evidence-based choices about health interventions. Their reviews are considered the gold standard of evidence-based medicine.
This is because most published meta-analyses simply report “statistically significant” conclusions. However, statistics can be misleading. As Mark Twain said: “There are lies. There are damn lies. And then there are statistics”.
The problem is the authors of most meta-analyses group studies together without considering the quality of studies included in their analysis. This creates a “Garbage In – Garbage Out” effect. If the quality of individual studies is low, the quality of the meta-analysis will also be low.
The Cochrane Collaboration reviews are different. They also report statistically significant conclusions from their meta-analyses. However, they carefully consider the quality of each individual study in their analysis. They look at possible sources of bias. They look at the design and size of the studies. Finally, they ask whether the conclusions are consistent from one study to the next. They clearly define the quality of evidence that backs up each of their conclusions.
For omega-3s and pregnancy, the Cochrane Collaboration performed a meta-analysis and review of 70 randomized controlled trials that compared the effect of added omega-3s on pregnancy outcomes with the effect of either a placebo or no omega-3s. These trials included almost 19,927 pregnant women.
This Cochrane Collaboration Review looked at all the claims for omega-3s and pregnancy outcome, but they concluded that only two of the claims were supported by high-quality evidence:
- Omega-3s reduce the risk of preterm births.
- Omega-3s reduce the risk of low birth-weight infants.
The authors concluded: “Omega-3 supplementation during pregnancy is an effective strategy for reducing the risk of preterm birth…More studies comparing [the effect of] omega-3s and placebo [on preterm births] are not needed at this point.”
of preterm birth…More studies comparing [the effect of] omega-3s and placebo [on preterm births] are not needed at this point.”
In other words, they are saying this conclusion is definite. The Cochrane Collaboration has declared that omega-3 supplementation should become part of the standard of medical care for pregnant women.
However, the Cochrane Collaboration did say that further studies were needed “…to establish if, and how, outcomes vary by different types of omega-3s, timing [stage of pregnancy], doses [of omega-3s], or by characteristics of women.”
That’s because these variables were not analyzed in this study. The study included clinical trials:
- Of women at low, moderate, and high risk of poor pregnancy outcomes.
- With DHA alone, with EPA alone, and with a mixture of both.
- Omega-3 doses that were low (˂ 500 mg/day), moderate (500-1,000 mg/day), and high (> 1,000 mg/day).
I have discussed these findings in more detail in a previous issue of “Health Tips From The Professor”
How Was This Study Done?
 The current study (SE Carlson et al, EClinicalMedicine, 2021) is a first step towards answering those questions.
The current study (SE Carlson et al, EClinicalMedicine, 2021) is a first step towards answering those questions.
The authors of this study focused on how much DHA supplementation is optimal during pregnancy. This is an important question because there is currently great uncertainty about how much DHA is optimal:
- The American College of Obstetrics and Gynecology recommends supplementation with 200 mg/day of DHA. However, that recommendation assumes that the increase will come from fish and was influenced by concerns that omega-3-rich fish are highly contaminated with heavy metals and PCBs.
- Another group of experts was recently asked to develop guidelines for omega-3 supplementation during pregnancy. They recommended pregnant women consume at least 300 mg/day of DHA and 220 mg/day of EPA.
- The WHO has recommended of minimum dose of 1,000 mg of DHA during pregnancy.
- Many prenatal supplements now contain 200 mg of DHA, but very few provide more than 200 mg.
Accordingly, the authors took the highest and lowest recommendations for DHA supplementation and asked whether 1,000 mg of DHA per day was more effective than 200 mg of DHA at reducing the risk of early preterm births. Their hypothesis was that 1,000 mg of DHA would be more effective than 200 mg/day at preventing early preterm births.
This study was a multicenter, double-blind, randomized trial of 1032 women recruited at one of three large academic medical centers in the United States (University of Kansa, Ohio State University, and University of Cincinnati).
- The women were ≥ 18 years old (average age = 30) and between 12 and 20 weeks of gestation when they entered the study.
- The breakdown by ethnicity was 50% White, 22% Black or African American, 22% Hispanic, 6% Other.
- 18% had a prior preterm birth (<37 weeks) and 7% had a prior early preterm birth (<34 weeks).
- Prior to enrollment in the study 47% of the participants reported taking a DHA supplement and 19% of the participants took a DHA supplement with > 200 mg/day.
All the participants received 200 mg DHA capsules and were told to take one capsule daily. The participants were also randomly assigned to take 2 additional capsules that contained a mixture of corn and soybean oil (the 200 mg DHA/day group) or 2 capsules that contained 400 mg of DHA (the 1,000 mg DHA/day group). The capsules were orange flavored so the participants could not distinguish between the DHA capsules and the placebo capsules.
Blood samples were drawn upon entry to the study and either just prior to delivery or the day after delivery to determine maternal DHA status.
The study was designed to look at the effect of DHA dose (1,000 mg or 200 mg) on early preterm birth (<34 weeks), preterm birth (<37 weeks), low birth weight (< 3 pounds), and several other parameters related to maternal and neonatal health.
How Much Omega-3 Should You Take During Pregnancy?
 The primary findings from this study were:
The primary findings from this study were:
- The rate of early preterm births (<34 weeks) was less (1.7%) for pregnant women taking 1,000 mg of DHA/day compared to 200 mg/day (2.4%).
- The rate of late preterm births (between 34 and 37 weeks) was also less for women taking 1,000 mg of DHA/day compared to 200 mg/day.
- Finally, low birth weight and the frequency of several maternal and neonatal complications during pregnancy, delivery, and immediately after delivery were also lower with 1,000 mg/day of supplemental DHA than with 200 mg/day.
This confirms the authors’ hypothesis that supplementation with 1,000 mg/day of DHA is more effective than 200 mg/day at reducing the risk of early preterm births. In addition, this study showed that supplementation with 1,000 mg of DHA/day had additional benefits.
This study did not have a control group receiving no DHA. However:
- The US average for early preterm births is 2.74%.
- For the women in this study who had previous pregnancies, the rate of early preterm birth was 7%.
Of course, the important question for any study of this type is whether all the women benefited equally from supplementation. Fortunately, this study was designed to answer that question.
As noted above, each woman was asked whether they took any DHA supplements at the time they enrolled in the study, and 47% of the women in the study were taking DHA supplements when they enrolled. In addition, the DHA status of each participant was determined from blood samples taken at the time the women were enrolled in the study. When the authors split the women into groups based on their DHA status at the beginning of the study:
- For women with low DHA status the rate of early preterm births was 2.0% at 1,000 mg of DHA/day versus 4.1% at 200 mg of DHA/day.
- For women with high DHA status the rate of early preterm births was around 1% for both 1,000 mg of DHA/day and 200 mg of DHA/day.
In other words, DHA supplementation only appeared to help women with low DHA status. This is good news because:
- DHA status is an easy to measure predictor of women who are at increased risk of early preterm birth.
- This study shows that supplementation with 1,000 mg of DHA/day is effective at reducing the risk of early premature birth for women who are DHA deficient.
In the words of the authors, “Clinicians could consider prescribing 1,000 mg DHA daily during pregnancy to reduce early preterm birth in women with low DHA status if they are able to screen for DHA.”
Which Omega-3s Are Beneficial?
 DHA is the most frequently recommended omega-3 supplement during pregnancy.
DHA is the most frequently recommended omega-3 supplement during pregnancy.
It is not difficult to understand why that is.
- DHA is a major component of the myelin sheath that coats every neuron in the brain. [You can think of the myelin sheath as analogous to the plastic coating on a copper wire that allows it to transmit electricity from one end of the wire to the other.]
- Unlike other components of the myelin sheath, the body cannot make DHA. It must be provided by the diet.
- During the third trimester, DHA accumulates in the human brain faster than any other fatty acid.
- Animal studies show that DHA deficiency during pregnancy interferes with normal brain and eye development.
- Some, but not all, human clinical trials show that DHA supplementation during pregnancy improves developmental and cognitive outcomes in the newborn.
- Recent studies have shown that most women in the United States only get 60-90 mg/day of DHA in their diet.
Clearly, DHA is important for fetal brain development during pregnancy, and most pregnant women are not getting enough DHA in their diet. This is why most experts recommend supplementation with DHA during pregnancy. And this study suggests supplementation with 1,000 mg/day is better than 200 mg/day. However, two important questions remain:
#1: Is 1,000 mg of DHA/day optimal? The answer is, “We don’t know”. This study compared the highest recommended dose (1,000 mg/day) with the lowest recommended dose (200mg/day) and concluded that 1,000 mg/day was better than 200 mg/day.
But would 500 or 800 mg/day be just as good as 1,000 mg/day? We don’t know. More studies are needed.
#2: Can DHA do it all, or are other omega-3s also important for a healthy pregnancy? As noted above, the emphasis on supplementation with DHA was based on the evidence for a role of DHA in fetal brain development during pregnancy.
But is DHA or EPA more effective at preventing early preterm birth and maternal pregnancy complications? Again, we don’t know.
As noted above, the Cochrane Collaboration concluded that omega-3s were effective at reducing early preterm births but was unable to evaluate the relative effectiveness of EPA and DHA because their review included studies with DHA only, EPA only, and EPA + DHA.
This is an important question because the ability of the body to convert EPA to DHA and vice versa is limited (in the 10-20%) range. This means that if both EPA and DHA are important for a healthy pregnancy, it might not be optimal to supplement with a pure DHA or pure EPA supplement.
Based on currently available data if you are pregnant or thinking of becoming pregnant, my recommendations are:
- Chose a supplement that provides both EPA and DHA.
- Because the evidence is strongest for DHA at this time, chose an algal source of omega-3s that has more DHA than EPA.
- Aim for a dose of DHA in the 500 mg/day to 1,000 mg/day range. Remember, this study showed 1,000 mg/day was better than 200 mg/day but did not test whether 500 or 800 mg/day might have been just as good.
As more data become available, I will update my recommendations.
The Bottom Line
The Cochrane Collaboration recently released a report saying that the evidence was definitive that omega-3 supplementation during pregnancy reduced the risk of early preterm births. However, they were not able to reach a definitive conclusion on the optimal dose of omega-3s or the relative importance of EPA and DHA at preventing early preterm birth.
Most experts recommend that pregnant women supplement with between 200 mg/day and 1,000 mg/day of DHA.
A recent study asked whether 1,000 mg of DHA/day was better than 200 mg/day at reducing the risk of early preterm birth. The study found:
- The rate of early preterm births (<34 weeks) was less (1.7%) for pregnant women taking 1,000 mg of DHA/day than pregnant women taking 200 mg/day (2.4%).
- For women with low DHA status at the beginning of the study, the rate of early preterm births was 2.0% at 1,000 mg of DHA/day versus 4.1% at 200 mg of DHA/day.
- For women with high DHA status at the beginning of the study, the rate of early preterm births was around 1% for both 1,000 mg of DHA/day and 200 mg of DHA/day.
The authors concluded, “Clinicians could consider prescribing 1,000 mg DHA daily during pregnancy to reduce early preterm birth in women with low DHA status…”
There are two important caveats:
- This study did not establish the optimal dose of DHA. The study concluded that 1,000 mg/day was better than 200 mg/day. But would 500 or 800 mg/day be just as good as 1,000 mg/day? We don’t know. More studies are needed.
- This study did not establish the relative importance of EPA and DHA for reducing the risk of early preterm births. DHA is recommended for pregnant women based on its importance for fetal brain development. But is DHA more important than EPA for reducing the risk of early preterm births? Again, we don’t know. More studies are needed.
For more details about this study and my recommendations, read the article above.
These statements have not been evaluated by the Food and Drug Administration. This information is not intended to diagnose, treat, cure, or prevent any disease.
