How Can You Reduce Your Cancer Risk?
Author: Dr. Stephen Chaney
 We are facing a food crisis in this country. Big Food Inc is taking over our diet. Currently, 73% of our food supply is processed. And because these are manufactured foods, not real foods, they are 52% cheaper than the whole unprocessed foods we should be eating.
We are facing a food crisis in this country. Big Food Inc is taking over our diet. Currently, 73% of our food supply is processed. And because these are manufactured foods, not real foods, they are 52% cheaper than the whole unprocessed foods we should be eating.
And Big Food Inc has seduced us. They know our weaknesses. The foods they make are convenient and easy to prepare. They also know our bodies were created with an ingrained craving for sweet, salty, and fatty foods. These cravings served us well in prehistoric times, but in today’s world Big Food Inc has weaponized them. Their foods are designed to satisfy every craving. They have done their best to make their processed foods irresistible!
The result is no surprise. In 2018 (LG Baraldi et al, BMJ Open, 2018, 8(3) e020574 60% of the calories the Average American consumes came from processed foods, and the percentage has only increased since then.
This is alarming because higher consumption of processed foods has been linked to increased risk of obesity, diabetes, and all-cause mortality.
Some studies have suggested that higher consumption of processed foods may also be linked to increased risk of cancer. The authors of the current study (K Chang, eClinicalMedicine 2023;56: 101840) set out to test this hypothesis.
How Are Processed Foods Defined In This Study?
 Before I proceed with describing the findings of this study, I should probably contrast the common definition of processed foods with the current scientific definition of processed foods. The scientific community has recently developed something called “The NOVA food classification system” to describe the various levels of food processing.
Before I proceed with describing the findings of this study, I should probably contrast the common definition of processed foods with the current scientific definition of processed foods. The scientific community has recently developed something called “The NOVA food classification system” to describe the various levels of food processing.
The NOVA system categorizes foods into four groups according to the extent of processing they have undergone:
- Unprocessed or minimally processed foods.
-
- This category includes foods like fruit, vegetables, milk, and meat.
2) Processed culinary ingredients.
-
- This category includes foods you might find in restaurants or prepare yourself to which things like sugar, vegetable oils, butter, or cream were added in the preparation.
3) Processed foods.
-
- This category includes foods like canned vegetables, freshly made breads, and cheeses.
4) Ultra-processed foods.
-
- This category includes foods like soft drinks, chips, packaged snacks, most breakfast cereals, chicken nuggets & fish sticks, fast food burgers, hot dogs, and other processed meats.
The actual list is much longer, but you get the idea. What we call processed foods, scientists call ultra-processed foods. Since the term “ultra-processed foods” has not yet entered the popular vocabulary, I will use the term “processed foods” in describing the results of this study because it is more understandable to the average reader.
How Was This Study Done?
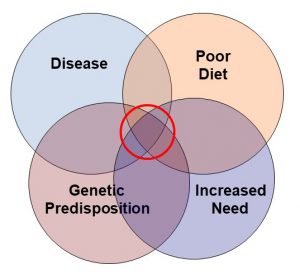
 The authors of this study started by using data from the UK Biobank study. The UK Biobank study is a long-term study in the United Kingdom that is investigating the contributions of genetics and environment to the contribution of disease.
The authors of this study started by using data from the UK Biobank study. The UK Biobank study is a long-term study in the United Kingdom that is investigating the contributions of genetics and environment to the contribution of disease.
The authors focused on 197,426 (54.6% women) participants in the study who completed up to five 24-hour dietary recalls between 2009 and 2012. The participants were age 58 (range 40 to 69) when they entered the study and were followed for an average of 9.8 years. None of the participants had been diagnosed with cancer at the time of their enrollment in the study.
The purpose of this study was to examine the correlation between percent of “processed food” in the participant’s diets and both the frequency of newly diagnosed cancer and the frequency of cancer deaths during the 9.8 years of follow-up.
More importantly, the size of this study allowed the authors to examine associations between processed food consumption and both the risk of cancer and cancer mortality for 34 site-specific cancers – something most previous studies were unable to do.
- The percentage “processed food” in their diets was calculated from the 24-hour dietary recalls using the NOVA scoring system.
- The frequency of newly diagnosed cancers and cancer deaths was obtained by linking the data in this study with the national cancer and mortality registries, provided by the National Health Service.
Do Processed Foods Cause Cancer?
 The authors started by dividing participants into four equal quartiles based on their consumption of processed foods:
The authors started by dividing participants into four equal quartiles based on their consumption of processed foods:
- For quartile 1 processed foods made up between 0 and 13.4% of calories (average = 9.2%).
- For quartile 2 processed foods made up between 13.5 and 20% of calories (average = 16.7%).
- For quartile 3 processed foods made up between 20.1 and 29.4% of calories (average = 24.3%).
- For quartile 4 processed foods made up between 29.5 and 100% of calories (average = 41.4%).
They started by looking at the risk of developing cancer during the 9.8-year follow-up period. A total of 15,921 participants developed cancer during that time. When the authors compared the group consuming the most processed foods with the group consuming the least processed foods:
- The risk of overall cancer of any type increased by 7%.
- The risk of lung cancer increased by 25%.
- The risk of ovarian cancer increased by 45%.
- The risk of diffuse large B-cell lymphoma increased by 63%.
- The risk of brain cancer increased by 52%.
Furthermore, every 10% increase in processed food consumption was associated with:
- A 2% increase in overall cancer incidence…and…
- A 19% increase in ovarian cancer incidence.
A total of 4,009 participants died from cancer during that time. When the authors compared the group consuming the most processed foods with the group consuming the least processed foods:
- Overall cancer mortality increased by 17%.
- Lung cancer mortality increased by 38%.
- Ovarian cancer mortality increased by 91%.
Furthermore, every 10% increase in processed food consumption was associated with:
- A 6% increase in overall cancer mortality.
- A 16% increase in breast cancer mortality.
- A 30% increase in ovarian cancer mortality.
The authors concluded, “Our UK-based study suggests that higher [processed food] consumption may be linked to an increased [frequency] and mortality for overall and certain site-specific cancers especially ovarian cancer in women…These findings suggest that limiting [processed food] consumption may be beneficial to prevent and reduce the modifiable burdens of cancer.”
How Can You Reduce Your Cancer Risk?
 Let’s start with the American Cancer Society recommendations to limit cancer risk:
Let’s start with the American Cancer Society recommendations to limit cancer risk:
1) Avoid tobacco use.
2) Get to and stay at a healthy weight.
If you are already at a healthy weight, stay there. If you are carrying extra pounds, try to lose some. Losing even a small amount of weight can reduce your risk of cancer and have other health benefits. It is a good place to start.
3) Be physically active and avoid time spent sitting.
Current recommendations are to get at least 150-300 minutes of moderate intensity or 75-150 minutes of vigorous intensity activity each week. Getting to or exceeding 300 minutes is ideal.
In addition, you should limit sedentary behavior such as sitting, lying down, watching TV, and other forms of screen-based entertainment. This is especially important if you spend most of your working day sitting.
4) Follow a healthy eating plan.
A healthy eating pattern includes a variety of vegetables, fiber-rich legumes (beans and peas), fruits in a variety of colors, and whole grains. It is best to avoid or limit red and processed meats, sugar-sweetened beverages, highly processed foods, and refined grain products. This will provide you with key nutrients in amounts that help you get to and stay at a healthy weight.
5) It is best not to drink alcohol.
It is best not to drink alcohol. People who choose to drink alcohol should limit their intake to no more than 2 drinks per day for men and 1 drink a day for women.
This study adds an exclamation point to the American Cancer Society’s recommendation to avoid or limit “processed meats, sugar-sweetened beverages, highly processed foods, and refined grain products”.
You may be asking, “What is so harmful about processed foods?” The most obvious harm is that they are replacing healthier foods that reduce cancer risk, such as “a variety of vegetables, fiber-rich legumes (beans and peas), fruits in a variety of colors, and whole grains” that the American Cancer Society recommends for reducing cancer risk.
But there are other reasons as well. In the words of the authors:
- “Evidence has been accumulating on the strong obesity and type-2 diabetes-promoting potential of [processed foods], both of which are risk factors for many cancers including those of the digestive tract and some hormone-related cancers in women.
- Emerging research has suggested other common properties of [processed foods] that may contribute to adverse cancer outcomes, including the use of controversial food additives, contaminants such as acrylamide that form during [food processing], and toxic contaminants such as phthalates and bisphenol-F that migrate from food packaging [into the food].”
The Bottom Line
You probably know that processed foods are bad for you. But do processed foods cause cancer? A very large study (197,426 people followed for 9.8 years) suggests the answer to that question appears to be yes.
When the authors of the study compared the group consuming the most processed foods with the group consuming the least processed foods:
- The risk of overall cancer of any type increased by 7%.
- The risk of lung cancer increased by 25%.
- The risk of ovarian cancer increased by 45%.
- The risk of diffuse large B-cell lymphoma increased by 63%.
- The risk of brain cancer increased by 52%.
And when they looked at cancer deaths and did the same comparison:
- Overall cancer mortality increased by 17%.
- Lung cancer mortality increased by 38%.
- Ovarian cancer mortality increased by 91%.
The authors concluded, “Our study suggests that higher [processed food] consumption may be linked to an increased [frequency] and mortality for overall and certain site-specific cancers especially ovarian cancer in women…These findings suggest that limiting [processed food] consumption may be beneficial to prevent and reduce the modifiable burdens of cancer.”
These results are alarming because the most recent study shows that 60% of calories in the American diet comes from processed foods, and the percentage is increasing each year. We need to reverse this trend!
For more information on this study, why processed foods increase your risk of cancer, and what the American Cancer Society recommends to reduce your risk of cancer, read the article above.
These statements have not been evaluated by the Food and Drug Administration. This information is not intended to diagnose, treat, cure, or prevent any disease.
____________________________________________________________________________
My posts and “Health Tips From the Professor” articles carefully avoid claims about any brand of supplement or manufacturer of supplements. However, I am often asked by representatives of supplement companies if they can share them with their customers.
My answer is, “Yes, as long as you share only the article without any additions or alterations. In particular, you should avoid adding any mention of your company or your company’s products. If you were to do that, you could be making what the FTC and FDA consider a “misleading health claim” that could result in legal action against you and the company you represent.
For more detail about FTC regulations for health claims, see this link.
https://www.ftc.gov/business-guidance/resources/health-products-compliance-guidance